
by Editor | Jun 23, 2016 | Ovulation, Perimenopause, Research
Jerilynn C. Prior BA, MD; Professor of Medicine/Endocrinology at the University of British Columbia; Scientific Director of the Centre for Menstrual Cycle and Ovulation Research When and why did you join the Society for Menstrual Cycle Research? I joined SMCR at the...
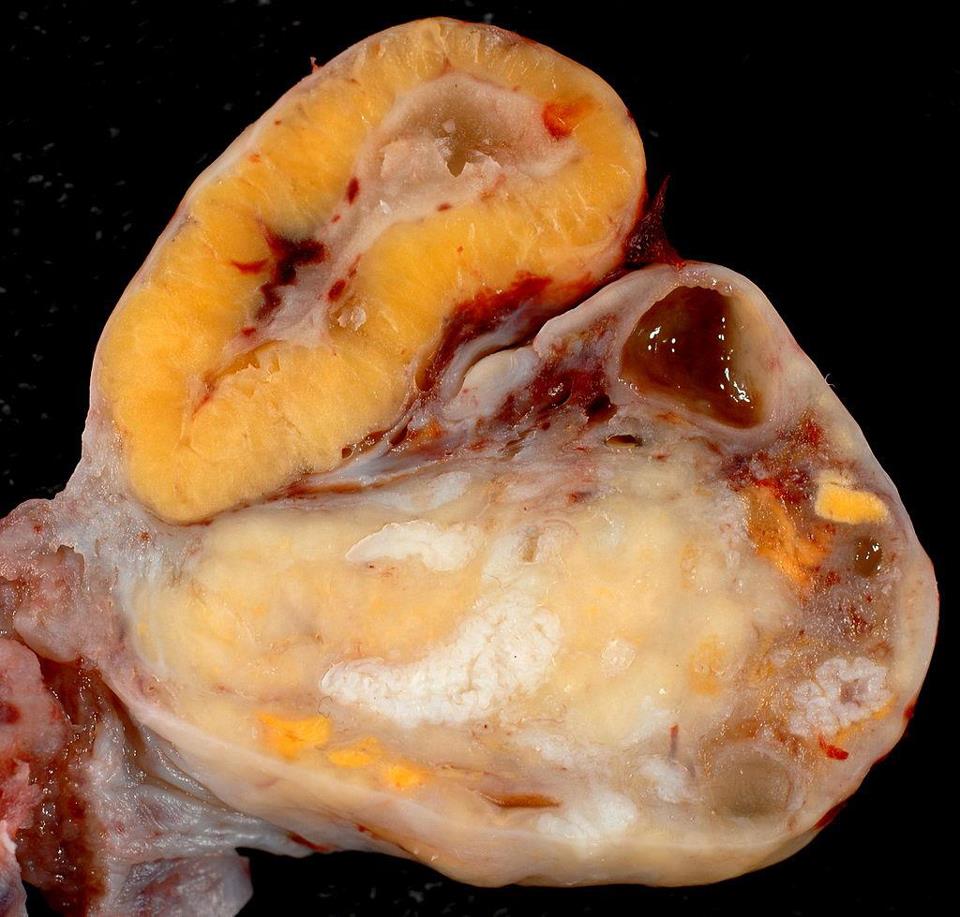
by Laura Wershler | Jul 23, 2015 | Ovulation
Everybody seems to be talking about ovulation these days in one context or another. ScienceDaily reported that women’s faces get redder when they ovulate, but it is imperceptible to the human eye. The Pharmaceutical Journal reported on a small study that showed...
by Editor | Jul 11, 2015 | FemCare, Ovulation, Reusable menstrual products
1. Naturopathic Doctor Lara Briden explains 4 Causes of Androgen Excess in Women on her Healthy Hormone Blog this week. If you are experiencing hair loss, facial hair (hirsutism) or acne, or have been diagnosed with PCOS, you’ll want to check this out for a...
by Laura Wershler | Jul 4, 2015 | Activism, Birth Control, Books, FemCare, Independent Film, Menstruation, New Research, Ovulation, Radio
Sweetening the Pill, the documentary Ricki Lake and Abby Eptsein are set to produce and direct, met it’s Kickstarter campaign goal on Friday, July 3rd, 2015, raising $119, 884 from 1750 backers to give the project the green light. The documentary was inspired by...
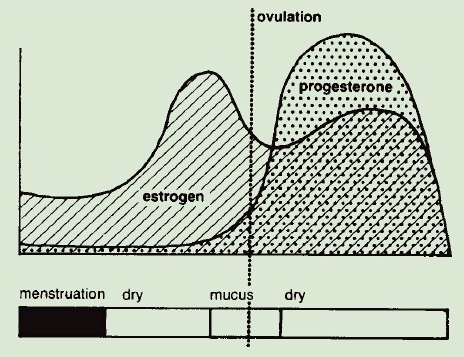
by Laura Wershler | Mar 27, 2015 | Literature, Menstruation, Ovulation, Reproduction
In Parts 1 and 2, I wondered why author Ann Patchett chose not to include information about menstruation, femcare products and birth control that, logically, would have enhanced her novel’s inciting premise—lifelong menstruation and fertility—while retaining the...
by Saniya Lee Ghanoui | Feb 2, 2015 | Art, Menstruation, Ovulation, Sports
Guest Post by Dana Michelle Gillespie Editor’s Note: This blog cross-posted from Pole World News. Pole dancing has quickly become one of the most internationally sought after fitness, sports, and art forms in the world. The pole movement craze is a rapidly...





