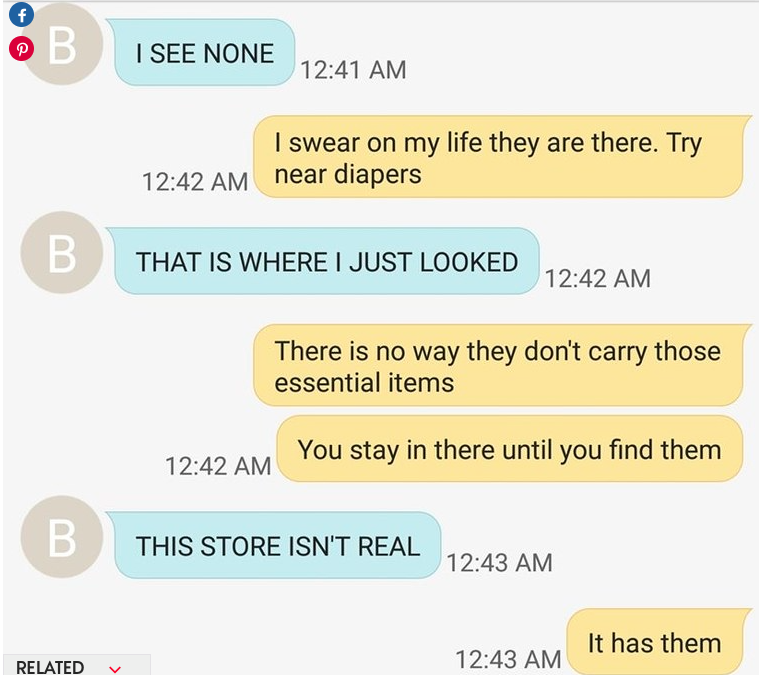
by Sophie Zivku | Oct 12, 2016 | Activism, Communication, Menstrual education, New Research
This fall, the plethora of menstrual-related news articles and social media trends is proving that we are well into what some may call a menstrual talk revolution. Menstrual discourse is no longer taking place in hushed tones behind closed doors. People are talking...

by Editor | Jun 29, 2016 | Communication, Literature, Research
David Linton, Ph.D., Professor Emeritus, Marymount Manhattan College When and/or why did you join the Society for Menstrual Cycle Research? As a scholar of communication and symbolic meaning, the social/cultural construction of the menstrual cycle is the most...
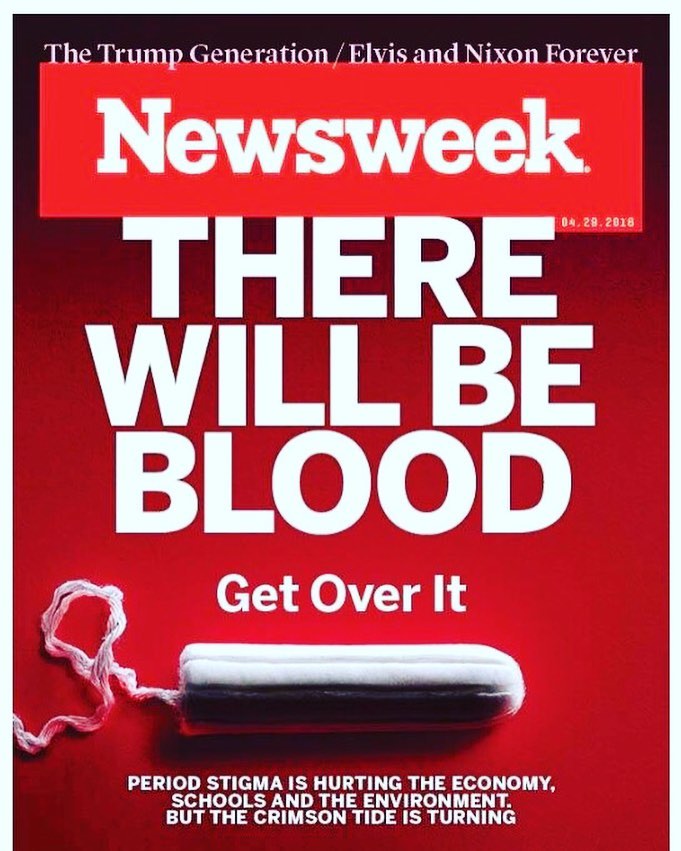
by Editor | May 31, 2016 | Communication, Media
Giuliana Serena critiques Newsweek’s period stigma cover story Note: This piece was first published on MoontimeRising.com. It has been edited for length for this repost at Menstruation Matters. I was pleasantly surprised and cautiously optimistic when I caught...

by David Linton | May 12, 2016 | Comedy, Communication, Media, Music, Television
It used to be that menstrual humor amounted to men making crass remarks about PMS and the world of stand up comedy was dominated by male performers. Well, not any more. In the last few years there seems to have been an explosion of young women comics doing stand-up...

by Jen Lewis | Jul 1, 2015 | Activism, Art, Communication, Media
Guest Post by Jen Lewis Beauty in Blood Presents Ms. July: Truth & Perception Year: 2015 Menstrual Designer: Jen Lewis Photographer: Rob Lewis...

by Editor | May 29, 2015 | Communication, Men, Menstruation, New Research
Menstrual musings on period cravings, talking about periods, contagious periods, communicating about periods, and what men know about periods will be presented in two concurrent sessions at the 21st Biennial Conference of the Society for Menstrual Cycle Research at...








